You may receive a 1095 form this year and wonder what to do with it. These forms are common when your insurance situation changes. That includes moving to marketplace coverage, leaving a job, or offering benefits through your business. Each version of the form serves a different purpose.
They look similar, but they are not the same. Using the wrong one or ignoring it could lead to missed credits or inaccurate filings.
This article explains what each version means, who gets it, and how it affects your taxes. For each form, you will find sections labeled “What We Like” and “What We Don’t Like” to help you understand how to use these forms effectively.
|
Form Type
|
Who Gets It
|
Purpose
|
Tax Impact
|
Filing Requirement
|
|
1095-A
|
Marketplace insurance holders
|
Premium tax credit reconciliation
|
Direct effect on tax liability
|
Required to file taxes
|
|
1095-B
|
Individual coverage, small employers, government programs
|
Proof of Coverage
|
Documentation only
|
Not required for federal filing
|
|
1095-C
|
Large employer (50+ employees) coverage
|
ACA compliance proof
|
Affects credit eligibility
|
Not required for federal filing
|
Now, let's dive into each form and what you need to know about it.
Contents |
| Form 1095-A: Marketplace Coverage |
| Form 1095-B: Proof of Coverage |
| What is a Form 1095-C, and Who Will Receive It? |
| Can I Get More Than One of These Forms? |
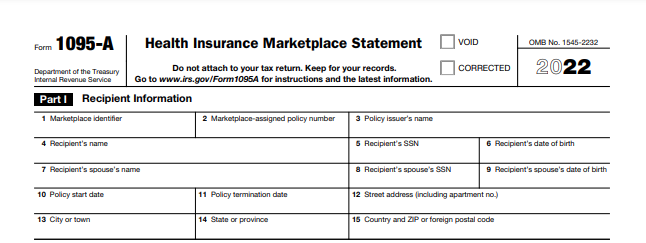
Form 1095-A: Marketplace Coverage
This form comes from the health insurance marketplace when you purchase coverage through a state or federal exchange. It includes coverage details and any advance premium tax credits you received.
What We Like
- Lists the months you had coverage and how much credit you received
- Required to complete Form 8962 for credit reconciliation
- Can increase your refund if your income ended up lower than expected
- Includes silver benchmark plan data to help calculate the final credit
What We Don’t Like
- You cannot file your tax return without this form
- Errors or delays may stall your return
- The form is often late and easy to misplace
- If your actual income is higher than projected, you may owe money back
Example: A business owner estimated $45,000 in income and received $4,800 in credits. Her actual income was $65,000. She qualified for only $3,600. She had to repay $1,200. The 1095-A showed what she needed to complete Form 8962.
What to Do When It Arrives
- Make sure the numbers match your marketplace account
- Download it online if the mailed copy has not arrived
- Request a correction if there is an error
- Set aside funds if your income was higher than expected
When Will You Receive 1095-A?
- Deadline: January 31
- Actual Timing: Often in February or early March
- How You’ll Get It: Usually electronic unless you request a paper copy
- Corrections: May be sent as late as March
If the form is missing:
- Log in to your marketplace account
- Contact customer service by mid-February if it is still unavailable
- Consider filing an extension if needed
Note: If you had marketplace insurance for part of the year, that is all the form will show.
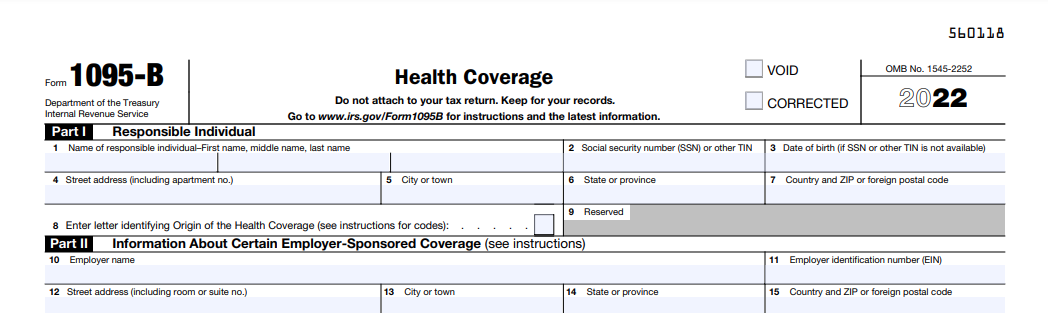
Form 1095-B: Proof of Coverage
This form verifies you had health insurance. You might receive it from a private insurance provider, a small employer, or a government program like Medicare.
What We Like
- Simple format with no calculations
- Applies to different plan types, including government programs and small group coverage
- Helpful for state-level reporting where required
- Less paperwork than marketplace forms
What We Don’t Like
- No financial information or tax credit data
- You might get it after other year-end documents
- Can create confusion if you also receive a 1095-A or 1095-C
- Not useful for federal tax planning
How It Differs from 1095-A
- Purpose: Documents coverage only, no credit tracking
- Tax Impact: None for federal returns
- Financial Info: Not included
- Filing Requirement: Not required for federal filing
Example: You own a small consulting firm and purchase insurance directly from an insurer. Each employee gets a 1095-B with their coverage dates. The form confirms insurance but does not show credit amounts or premiums.
What to Do with This Form
- Save it with your tax records for at least three years
- If you live in a state with an individual mandate, keep a digital copy
- Check for coverage gaps in case you apply for marketplace coverage later
When Should I Expect to Get a Form 1095-B?
- Deadline: March 31
- Private Insurers: Often send by January 31
- Government Programs: May take longer
- Small Employers: Usually send with W-2s and other year-end documents
Reminder: You do not need this form to file your federal return, but it may be required by your state.
State Considerations: Some states maintain individual mandate penalties, including California, Massachusetts, New Jersey, Rhode Island, Vermont, and Washington D.C. If you live in these areas, your 1095-B provides crucial compliance documentation to avoid state tax penalties, which can range from several hundred to over a thousand dollars depending on the state.
Record-Keeping Strategy: Keep these forms for at least three years. While not needed for current federal tax filing, they provide valuable coverage history for IRS audits, insurance applications, or future coverage transitions.
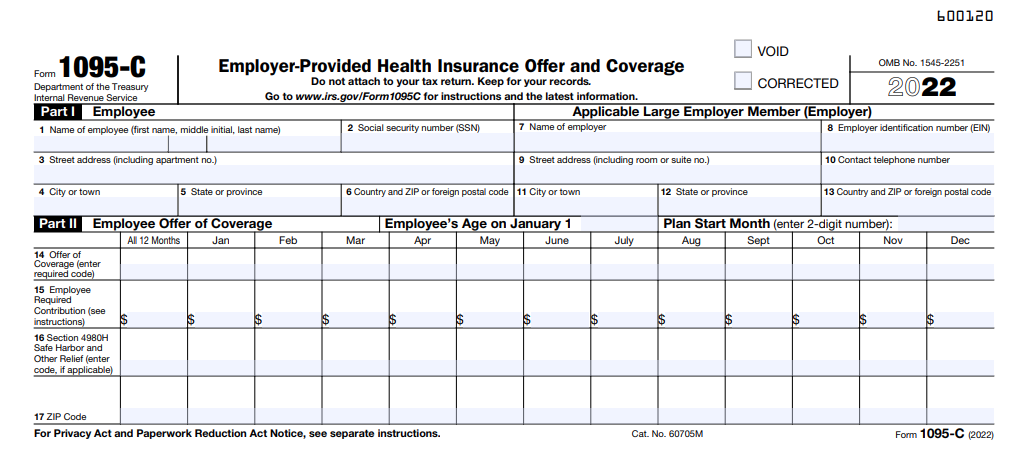
What is a Form 1095-C, and Who Will Receive It?
This form comes from businesses with 50 or more full-time equivalent employees. It shows what health insurance options were offered and whether you enrolled.
What We Like
- Confirms employer met ACA affordability and coverage standards
- Useful for credit eligibility if you declined employer coverage
- Helps document appeals or disputes with the marketplace
What We Don’t Like
- Includes technical codes that are hard to read
- Must be issued even if you declined coverage
- Creates compliance burden for employers
- May delay decision-making for employees
Who Uses This Form
- Employees: To understand what coverage was offered
- Employers: To prove ACA compliance
For Business Owners: If your company has 50 or more full-time equivalent employees, you must issue 1095-C forms and file them with the IRS. Late or missing forms may trigger penalties of $280 per form. Intentional disregard increases the fine to $570.
How to Prepare
- Track employee status and offers month by month
- Coordinate with payroll to report correct data
- Understand affordability formulas such as the federal poverty line and W-2 safe harbors
- Keep documentation for at least three years
When Will I Get a Form 1095-C?
- Employee Copy Deadline: January 31
- IRS Filing (Paper): February 28
- IRS Filing (Electronic): March 31
- Extensions: Available with proper filing
Note: You will receive the form even if you declined coverage. Contact your HR department if the information is incorrect.
Business Owner's 1095-C Action Plan:
- If Issuing Forms: Start gathering employee data by December 1st
- If Receiving Forms: Compare offered coverage costs to marketplace alternatives
- Documentation: Keep copies for potential premium tax credit claims
Cost Reality Check: For business owners issuing these forms, expect $500-$750 in preparation fees for 100 employees, plus potential penalties for missed deadlines. Many businesses use specialized software or outsource to avoid compliance risks.
Can I Get More Than One of These Forms?
Yes. Many business owners and employees receive more than one of these forms during coverage transitions.
Examples
- Corporate Restructure: Started the year with 1095-C, moved to 1095-A after downsizing
- Dual Role: You use marketplace insurance personally but offer group coverage to employees
- Job Change: You left a large employer mid-year and enrolled in a marketplace plan
What We Like
- Provides full coverage documentation
- Helps with accurate tax filings
- Supports strategic planning
What We Don’t Like
- Increases paperwork and complexity
- Makes it easier to miss something important
- Requires extra time for review and organization
How to Stay Organized
- Create a calendar that shows which type of coverage applied each month
- Separate forms by whether they affect your tax filing
- Hire a tax professional if you’re unsure how to handle multiple forms
Note: The 1095-A is required to reconcile premium tax credits. The 1095-C affects your eligibility to receive them.
The Bottom Line
These forms can be confusing, but they affect your taxes and your business. At DiMercurio Advisors, we help business owners stay compliant while making smart insurance decisions that support long-term goals.
What You Get with Our Help
- Accurate review of all 1095 forms
- Integrated tax and coverage planning
- Help avoiding costly compliance mistakes
- Coordination based on your business structure
Premium tax credits, ACA compliance, and employee health plans all connect back to your tax strategy. With our help, you can avoid errors and uncover savings you may have missed.
If you’re unsure how these forms affect your situation, talk to our team. We’ll help you file correctly and make confident decisions for your business and your future.